A $30,000 grant will establish a faculty research fund at CIIS, creating opportunities for innovative studies in Somatic Psychology and Integral and Transpersonal Psychology.
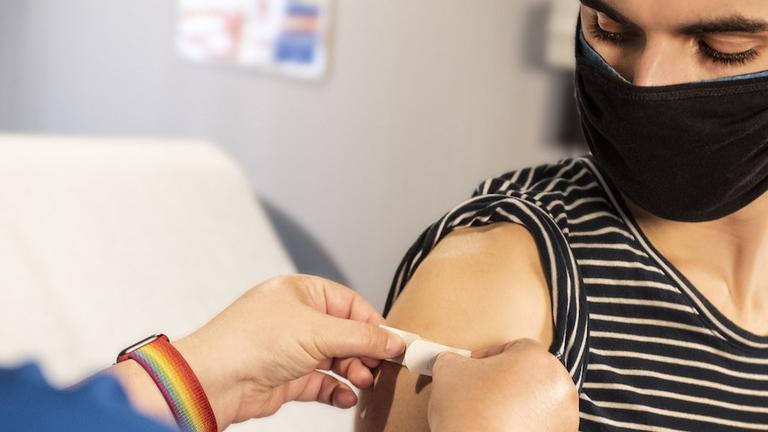
The Shot That Keeps Giving
Chair of the Integrative Health Program, Meg Jordan, describes her experience as an early COVID-19 testing clinician and vaccine administrator
As an active licensed RN and member of the Marin Medical Reserve Corp, I’ve undergone specialized training to offer COVID-19 vaccine injections for the Department of Health and Human Services. This is a story of that experience, starting on Dec 23, 2020, when I was teamed with three other RNs, one paramedic, and public health officials to provide some of the first injections to the health care staff at a nearby skilled nursing facility (SNF).
All summer I had served as a COVID case investigator, and contact tracer, and then started testing for COVID, performing all three types of swabs--nasopharyngeal, mid-turbinate, and anterior nares---following more hours of training. To do this specialized work, you have to be test-fitted with n95 masks and be sprayed in the face with a noxious-smelling gas to see if you can taste it on your tongue, which would indicate a leak in the mask. If that happens, you try another mask. You also have to learn the updated protocol for wearing protective gear (PPE), including gowns that wrap around you, fit-tested masks, face shields, hair covers, booties, and double gloving. I’ll be grateful to the County public health directors who made sure that vaccinators and testers were as protected as possible.
Our team met a few days before Christmas at the SNF only to find that the staff had no idea we were coming, and were unprepared for us. County public health departments are notoriously underfunded, and with all last minute, urgent activity of this pandemic, it’s no wonder that a few phone calls and notifications are missed. But the SNF director scrambled and we pulled the clinic together.
Because the facility was a hot zone with an active COVID outbreak, we had to give the injections in an outdoor courtyard, on a briskly cold day for 5-6 hours. We took no breaks because we didn’t want to don and doff our PPE, (that alone is a risk with an airborne virus) so that meant, no lunch, no drinks, no bathroom. We borrowed folding tables and quickly went about sterile wiping everything down, including a dozen chairs, while we set up four stations: one for registration and counseling, two vaccination tables, and one recovery area, where people were observed for 15-25 minutes for possible adverse reactions or anaphylaxis. I noted how smoothly my RN colleagues, all former or current ICU or ER nurses like myself, moved into action together, even though we never met till that morning. It was a familiar, no-nonsense rhythm of providing what was critically needed and a welcomed break from the social and political worries and obsessions I experience most days of these lockdowns.
A few words about this SNF: At first glance, it was dingy, bare-bones, rundown, and no doubt, housed very elderly people who felt discarded or forgotten. This was no Redwoods or Marin Villas, where more affluent residents are expected to hand over life savings and enjoy a highly trained and entertaining staff. Instead, there were folks at this SNF who had no place else to go, but the new Director of Nursing was determined to create a safer, more pleasant ending to their lives. She had arrived at a poorly managed site, and was cleaning it up, firing and hiring new staff, and creating order out of chaos. Her methods reminded me of Florence Nightingale’s two field medicines of basic hygiene and caring communication, and she told me she had actually fallen in love with the residents, and staff, and the experience injected new life into her long career. Well, all but one resident, who was a mentally unstable homeless woman who found an empty room and took up squatting rights ever since, spewing racist vitriol and ransacking a few rooms. They were at a loss on how to move her out. No agency would take her, and she observed our daylong clinic from her window.
You might wonder if we were there to vaccinate the frail elderly residents. No, just the staff. California follows the CDC recommendations to first vaccinate the most at-risk which aren’t the non-ambulatory 90-year-olds, but are the health care workers—the nursing aids, orderlies, cooks, cleaners, and janitors of nursing homes and SNFs. These folks are often new immigrants, people of color with higher rates of chronic disease, who work for low wages due to minimal education or lack of documentation. They work hard holding onto the only job they could get without specialized credentials, and they do their best in the poorest of conditions. They are most at-risk from an epidemiological viewpoint, taking public transit back and forth to crowded living conditions, frequenting stores or working extra shifts at essential service jobs, in contact with hundreds of people each week, and also going room to room at the SNF, sometimes in more than one facility.
However, it wasn’t always easy to convince staff to receive a voluntary injection. While a few gladly rolled up their sleeves for the intramuscular deltoid injection, several were influenced by false information about the “lack of testing” or that “it gives you the disease.” One worker told me he heard about the deplorable, unethical Tuskegee experiments on Black men that monitored their untreated syphilis. I spent a lot of time listening to his fears, acknowledging the deceitful practices that marginalized people have undergone, and slowly earning his trust. He helped to see the entire rest of the staff finally line up, and by the end of the day, he came in to get his own injection, but warned us that “if I die, I’m gonna sue y’all.” The deal was made.
When the public health official arrived with the refrigerated case of Pfizer-BioNTech COVID-19 vaccine, we gathered around to open the first box. I can’t emphasize enough how emotional this moment was for all of us. We beheld the rows of tiny purple-capped vials, and a wave of emotion swept over the entire team. Maybe because these were among the first vaccines to arrive in Marin County, maybe because it was the day before Christmas Eve, and we were huddled together on a bone-chilling cold day in an SNF courtyard strung with paper Christmas decorations and a few cheery lights, but there was no denying that we felt like something precious and rare and long sought after was in our hands. It was viewed as a very privileged and sacred moment, a chance to end this epidemic of sickness, death, and loneliness. I gingerly picked up one vial with a double-gloved hand and joked, “Look at us, we look like we’re gazing at baby Jesus as if a Christmas miracle had arrived!” And true to form, we bust out laughing, a typical response of emergency personnel to break the tension and get back to work.
We managed to warm the vials to room temperature, tracked the lot numbers, reconstituted them with 1.8 mL of 0.9% preservative-free saline, and drew up the .3 mL amounts in separate syringes. We then vaccinated the entire staff present, and even a few who had the day off, but took hours of busses to come back for their jab. At the end of the shift, once everyone received the vaccine, we called the public health officers to say we had enough left over in the vials (Pfizer really does provide almost 6-7 doses, more than the stated 5), and got permission to inoculate each other, another moment of deep gratitude. I was surprised that this injection left no heavy-arm feeling, nor did I have any flu-like symptoms the next day.
I’ve since been scheduled to do more vaccinator shifts this month, as my teaching schedule allows, and it’s exciting to give them to this wider population of 16 and over. While most people I talk with are thrilled to know that the vaccine is slowly making its way to to everyone, there are still those who are fearful of its safety, and in those cases, I offer this moment of mindful reframing.
Consider transmuting that fear with the current fact-based reality, that the world is participating in a massive, coordinated effort to bring a remarkable mRNA breakthrough vaccine to everyone who needs it. It’s the brilliant culmination of the work of thousands of people--scientists, virologists, clinical investigators of RCTs, immunologists, epidemiologists, refrigerant engineers, delivery and dissemination experts, independent medical advisory boards, government, and private enterprise partners, dedicated public servants, extraordinary public health leaders—and it is amazing that it winds up in the hands of volunteers like me willing to reach out and ask you to roll up your sleeve for a healthier, safer, happier world than what we’ve known this past year.
Related News
Playwright and activist Alex Burger brings his global experience into the CIIS MFA classroom, teaching art as transformation, and crisis as creative fuel.
Fernando Ona, Chair of Transformative Inquiry at CIIS, carried questions from Iraq to the classroom—and found space to explore them.



